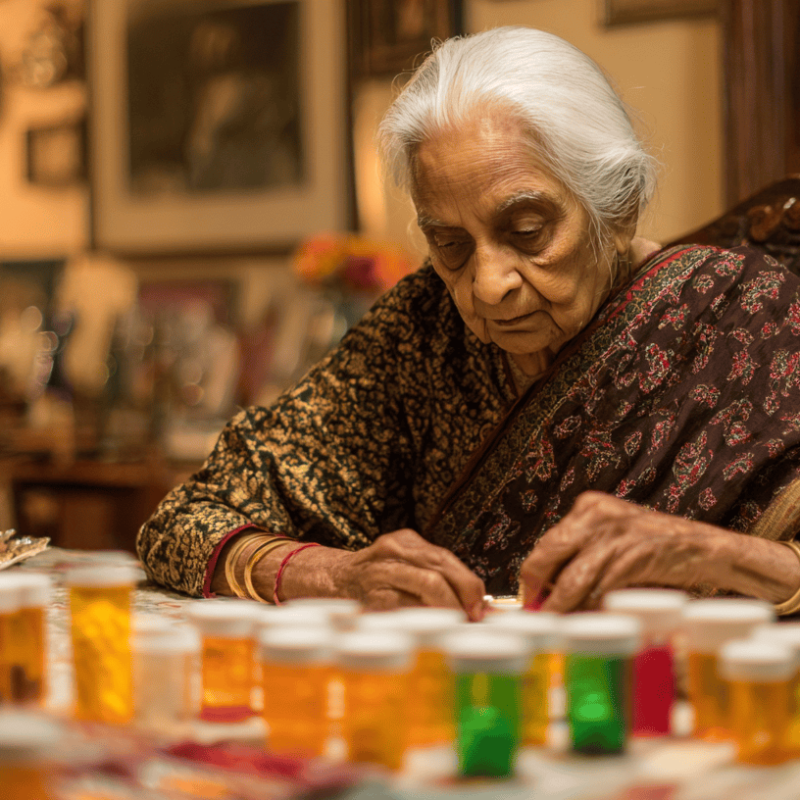Managing multiple medications can feel like running a small kitchen — every item has its own timing, rules, and storage needs. One is “with food,” another is “on an empty stomach,” and a third is “as needed,” but only sometimes. It’s a lot to hold in your head.
If you’ve felt stressed, tired, or afraid of making a mistake, you’re not alone. Managing multiple medications is hard, even for organized people, because life isn’t perfectly routine.
The good news is that you don’t need a perfect memory. You need a clear list, a simple daily routine, and steady check-ins with your doctor and pharmacist. These steps work well for older adults, caregivers, and anyone living with chronic conditions. And if you want to check whether your medications are safe together, we built a free Medication Safety Scanner specifically for that — add your medications by photo or by hand and get a plain-language report in under a minute.
Start with a clear medication list you can trust

A reliable medication list is the base for everything else. It helps your doctor make safer choices, helps your pharmacist spot problems, and helps you feel less anxious day to day.
If you only do one thing this week, make your list accurate and easy to find.
📘 Download the free eBook Managing Multiple Medications Without Feeling Overwhelmed
Write down the essentials for each medicine
Think of your medication list like a map. If the map is wrong, you can end up in the wrong place, even if you follow it carefully.
For each prescription medicine, write down:
- Name: brand and generic (if you know both)
- Dose: for example, 10 mg
- How you take it: 1 tablet, 2 puffs, 5 mL
- When you take it: morning, bedtime, every 8 hours, or specific times
- Why you take it: blood pressure, pain, thyroid, sleep, mood
- Special instructions: with food, avoid grapefruit, don’t crush, take with water
- Prescriber: Dr. Patel, cardiology, primary care
- Pharmacy: name and phone number
Also add the items people often forget, even though they matter:
- Over-the-counter meds (antacids, allergy pills, stool softeners)
- Vitamins and herbals
- Eye drops and ear drops
- Inhalers and nebulizers
- Creams, patches, and ointments
- “As needed” meds (pain pills, nausea meds, nitroglycerin)
A practical setup is two copies:
- A paper copy at home (many people keep it on the fridge)
- A wallet card (folded paper is fine)
If you use a smartphone, a photo of the list can help. Paper still wins in an emergency.
Do a medication check after every change
Medication lists go out of date fast. A small change can ripple into confusion, especially after a hospital stay.
Update your list any time you:
- Start a new prescription
- Change a dose or schedule
- Stop a medicine
- Switch pharmacies
- Add a supplement, vitamin, or new over-the-counter product
- Leave the hospital or rehab (this is a common point for mix-ups)
A simple habit helps: after any appointment where meds change, pause before you leave and ask, “What changed, and why?” Write it down right away.
For appointments, consider a “brown-bag review.” Put all bottles (including eye drops, inhalers, vitamins) in a bag and bring them in. If that’s too heavy, take clear photos of the labels. Ask the clinician or pharmacist to compare what you take at home with what’s listed in the chart. That one step can prevent months of errors.
Build a simple daily routine that prevents missed doses
The goal is not to turn your day into a medication calendar. The goal is to make taking your meds feel like brushing your teeth, a steady habit that doesn’t take much thought.
Don’t change your dose or timing on your own. Build a routine around the directions you were given, then ask for help if it’s not working.
Match medication times to daily habits
Most people miss doses for one reason: the timing doesn’t fit their day. Anchoring your meds to habits you already do can cut missed doses fast.
Common anchors that work well:
- Breakfast: coffee, oatmeal, morning news
- Brushing teeth: morning and night
- Dinner cleanup: dishes, setting out tomorrow’s items
- Evening TV: the same show each night
- Bedtime: phone charger, light off, nightstand routine
Some meds have strict rules. You can still use anchors, you just choose the right ones.
- If a medicine must be taken on an empty stomach, you might anchor it to waking up, then take other morning meds with breakfast.
- If a medicine must be taken with food, pair it with the first bites of breakfast or dinner, not “sometime later.”
- If a medicine must be taken at a set time, use a clock-based reminder, then tie the follow-up action to something nearby (like the pill organizer next to your kettle).
Real life changes routines. Travel, guests, late meals, and appointments can throw off even the best plan. When your day shifts, keep one rule: don’t guess. Check the label and use your pharmacist as your back-up when you’re unsure.
Choose the right organizer and reminders
The right tools should match your vision, your hands, and your memory. The best organizer is the one you’ll actually use on a tired day.
Here’s a quick comparison:
| Tool | Best for | Watch-outs |
|---|---|---|
| Weekly pill box | Simple schedules, steady routines | Some pills need original bottles or special storage |
| Day-and-time organizer | Multiple daily doses | Tiny compartments can be hard with stiff fingers |
| Pharmacy blister packs | Many meds, caregiver support | Needs planning, changes can take time to update |
| Phone or smart-speaker alarms | People who keep a device nearby | Alarm fatigue, keep the message clear (“Take morning meds”) |
A few safety basics matter more than fancy features:
- Store meds away from heat and moisture (a steamy bathroom isn’t ideal).
- Keep them out of reach of kids and pets.
- If you use an organizer, keep original bottles for reference, refills, and label instructions.
- Don’t mix pills in a bowl or loose in a drawer. It’s an easy way to lose track.
Your pharmacist can often make daily life easier with small changes:
- Easy-open caps (if child-proof caps aren’t needed in your home)
- Large-print labels
- Color stickers to separate morning and evening meds
If you struggle to open bottles or read labels, say so. It’s a common issue, and pharmacies handle it every day.
Make your medications safer with your doctor and pharmacist

Overwhelm isn’t just about the number of pills. It often comes from unclear directions, side effects that feel scary, and meds that overlap after years of new diagnoses.
Your care team can help reduce confusion and improve safety, but they need clear information from you. Bring your medication list, bring questions, and speak up about what’s hard.
Never stop a medicine without medical advice. Some drugs must be tapered, and some protect you even when you don’t “feel” them working.
Download the Free eBook
📘 Managing Multiple Medications Without Feeling Overwhelmed
Ask for a simpler plan when you can
Many medication schedules can be simplified, but it takes a direct conversation. Bring a short question list to your next visit, especially if you’re taking several daily doses.
Helpful questions to ask:
- Can any of these be taken at the same time?
- Can any be taken once daily instead of twice daily?
- Do I have any duplicates that do the same job?
- Is there a combination pill that could replace two separate pills?
- Is there a lower-cost option that works as well?
- What is the goal of each medicine, and how will we know it’s helping?
For older adults, you may also hear the term deprescribing. This means a doctor-guided process of reducing or stopping medicines that no longer help, or that cause more harm than benefit. It isn’t about “giving up.” It’s about keeping the plan sensible as your body and needs change.
A simpler schedule often leads to better follow-through. Fewer daily dosing times usually means fewer missed doses.
Know the warning signs of side effects and interactions
Side effects can look like “just aging,” but sometimes they come from a medicine, or a mix of medicines. Pay attention when something changes soon after a new drug, a new dose, or a new supplement.
Red flags to take seriously include:
- Dizziness or feeling unsteady
- Falls or near-falls
- Confusion or new memory trouble
- Unusual sleepiness or trouble staying awake
- New stomach upset (nausea, vomiting, bad heartburn)
- Swelling in legs, feet, or face
- Rash or hives
- Bleeding or easy bruising
- New shortness of breath or chest discomfort
Interactions are another reason routines get scary. Alcohol can worsen sleepiness and raise fall risk with many medicines. NSAIDs like ibuprofen and naproxen can be risky for some people with kidney disease, ulcers, high blood pressure, or when combined with blood thinners. Sleep aids, including some over-the-counter products, can add confusion and unsteadiness.
One practical safety step: use one pharmacy when possible. When a new medicine is added, ask the pharmacist to check for interactions, including vitamins and herbals. It’s a quick request that can prevent serious problems.
Plan for real life, missed doses, refills, and emergencies

Even with a good routine, life will interrupt it. A missed dose does not mean you’ve failed. It means your system needs a back-up plan.
The goal here is calm and safe action, not guesswork.
Set up a refill system that prevents last-minute stress
Running out creates panic, and panic leads to mistakes. A refill system removes that pressure.
Strong options include:
- Syncing refills so prescriptions renew around the same time
- Auto-refill (when appropriate) and text or phone alerts
- Ninety-day supplies if your plan allows it and your doctor approves
- Mail delivery for those with mobility limits or no easy transport
A simple rule works well for most people: request refills when you have 7 to 10 days left. That cushion covers weekends, pharmacy delays, and prescriber approvals.
Cost stress also causes skipped doses. If cost is an issue, ask about:
- Generics
- Manufacturer assistance programs (your pharmacy may know what’s available)
- A medication review during Medicare Part D open enrollment (Oct 15 to Dec 7 each year), when many people can change plans
If it’s already December, put a reminder on your calendar for next year. Even small plan changes can lower costs.
Create a quick plan for missed doses and emergencies
Missed doses happen most often when you’re away from home, exhausted, or distracted. The safest response is boring and consistent.
- Read the prescription label first. Many labels include clear instructions.
- If the label isn’t clear, call your pharmacist or prescriber. Don’t double up unless a professional tells you to.
- If you’re helping a spouse or parent, write down what you did and when, so nobody has to guess later.
A few preparedness steps can save time in an urgent moment:
- Keep your current medication list on the fridge or another visible spot.
- Carry a small card with allergies, key conditions, and an emergency contact.
- If memory or vision is a challenge, consider caregiver check-ins, even if it’s a quick daily text or phone call.
Pill organizers can be helpful, but only if the person filling them can do it accurately. If that’s becoming hard, ask the pharmacy about blister packs or ask a family member to help with weekly set-up.
A Smarter Way to Check Your Medications at Home
One of the questions I hear most often from patients and their families is this: “How do I know if these medications are safe together?” It’s a fair question — and until recently, the honest answer was “call your pharmacist and hope you get a quick callback.”
We’ve built something to help with that right here on The Senior Living Report. Our Home Safety Scanner is a free AI-powered tool designed specifically for older adults and their caregivers. Right now it focuses on home safety — walking through your living environment and flagging potential hazards before they become problems.
But we’re building something bigger. The next feature in development is a medication safety scanner — a tool that will let you enter your medications and get an plain-language summary of potential interactions, timing conflicts, and red flags worth discussing with your doctor or pharmacist. Not to replace your healthcare team, but to help you walk into those conversations better prepared.
If that sounds like something you’d find useful, join our email list and you’ll be the first to know when it launches. In the meantime, the Home Safety Scanner is free and ready to use today — and for many older adults, what’s on the floor and in the hallway is just as important as what’s in the medicine cabinet.
Conclusion
Managing multiple medications can feel lighter when you rely on a few steady habits: one trusted medication list, one daily routine tied to your normal day, and regular reviews with your doctor and pharmacist. You don’t need to hold every detail in your head, you just need a system you can repeat.
Update your list today, even if it’s messy at first, then ask your pharmacist this week to review it for safety and interactions. A clearer plan means less worry, and a safer, calmer day with your medications.